The Emergency Hospitals Aren’t Prepared For

Hospitals are designed to withstand clinical emergencies.
What they’re often not designed to withstand is the failure of the systems that quietly keep care possible in the first place.
When a critical system like HVAC, steam, power, or building controls fails, the impact extends far beyond a repair invoice. It triggers a cascade of regulatory, clinical, operational, and financial consequences, many of which hospital leaders never see itemized on a balance sheet.
For healthcare executives navigating thin margins and rising scrutiny, this is no longer a facilities problem. It’s an enterprise risk.
The Moment a Critical System Fails, Costs Multiply
Critical infrastructure failures rarely stay contained. A single HVAC failure can quickly escalate into a multi-department disruption.
Common downstream impacts include:
- Operating rooms or ICUs taken offline due to temperature, humidity, or pressure violations
- Cancelled procedures and patient transfers
- Infection control exposure from inadequate air changes or humidity control
- Emergency rentals (chillers, temporary boilers) and premium contractor labor
- Staff overtime, burnout, and diverted clinical focus
Emergency repairs alone cost approximately 18% more than planned maintenance. Although those totals can add up quickly, that premium is often the smallest cost incurred.
Key takeaway: The visible repair cost is only the first line item in a much longer chain reaction.
Why These Failures Are Becoming More Likely
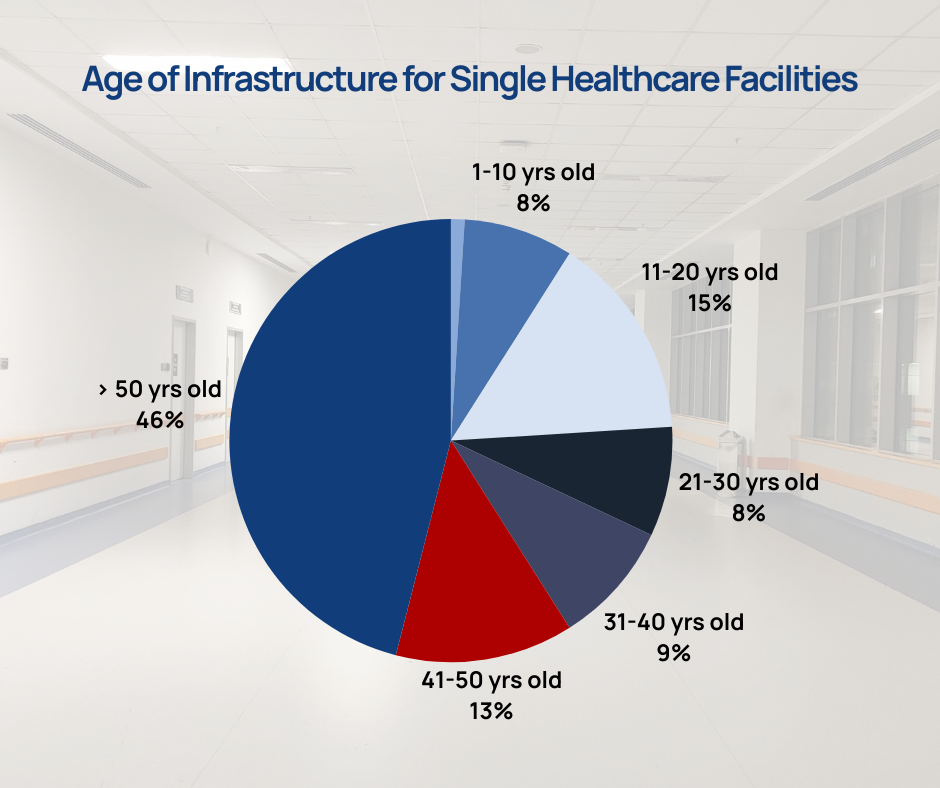
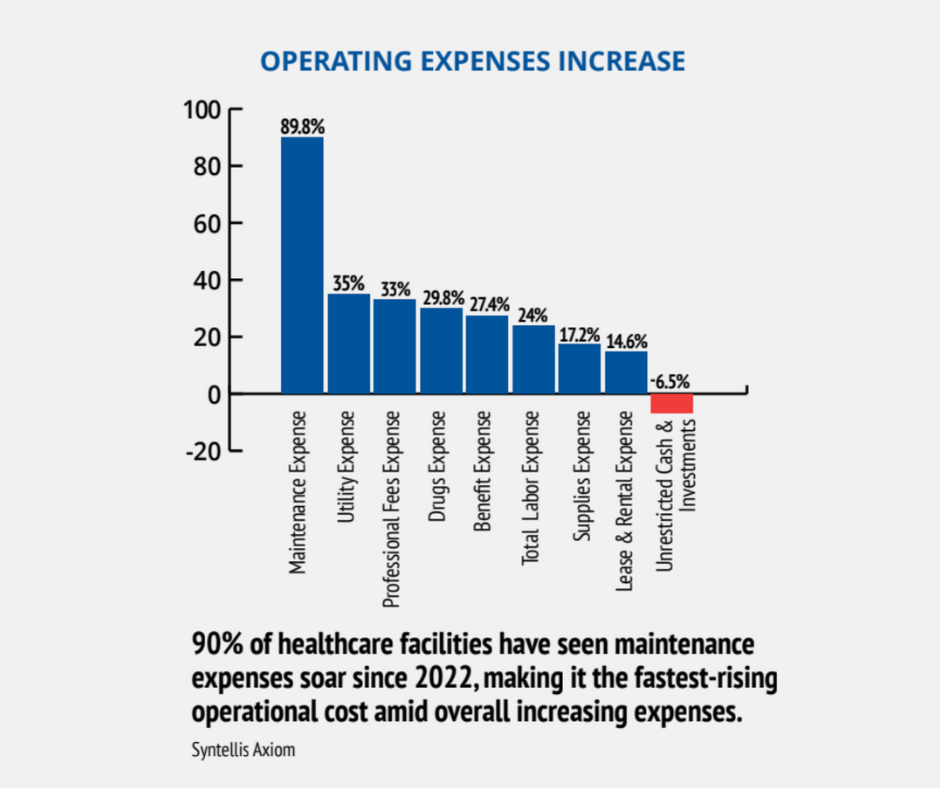
Many hospitals are operating critical systems that are technically “functional,” but no longer resilient.
According to the 2024 HFM Hospital Operations Survey, 68% of healthcare facilities operate infrastructure that is more than 30 years old. Aging systems often:
- Lack redundancy
- Operate outside optimal efficiency ranges
- Rely on manual oversight instead of automated fault detection
- Fail under peak demand, extreme weather, or clinical surges – the worst possible times
At the same time, hospital operating expenses are rising at more than 5% annually, with maintenance and utilities among the fastest-growing cost categories (Syntellis Axiom).
This creates a dangerous paradox:
- Deferring upgrades until the next year feels financially responsible in the short term
- But deferral increases the probability of catastrophic, unplanned failure
“Still running” is often the most dangerous status a critical system can have.
Compliance: The #1 Pain Point That Failure Exposes

For hospital leadership, compliance is a top concern.
Hospitals must continuously meet stringent requirements tied to:
- State healthcare boards
- CMS Conditions of Participation
- Environment of Care standards
- Accreditation surveys
When HVAC systems can’t maintain humidity, pressure, or air changes per hour in critical spaces, compliance gaps emerge immediately.
These gaps can result in:
- Accreditation citations
- Forced corrective action under compressed timelines
- Increased scrutiny from regulators and boards
- Potential lost revenue and staff frustration due to delayed or cancelled procedures
Poorly functioning building systems are one of the most common underlying contributors to compliance findings, according to healthcare facilities management data.
Compliance is not a separate risk from infrastructure; it is a direct outcome of it.
Patient Care and Staff Experience Are Directly Affected
Outside of regulatory exposure, infrastructure failures directly affect patient outcomes and staff morale.
The CDC estimates that 1 in 25 hospital patients is affected by a hospital-acquired infection (HAI) on any given day, and environmental conditions such as ventilation and humidity play a documented role in infection transmission.
Hospitals collectively receive hundreds of millions of dollars annually in Medicare reimbursement penalties tied to HAIs, according to CMS and HHS reporting.
At the same time:
- Inconsistent temperatures and air quality increase patient discomfort
- Manual system oversight adds workload to already stretched facilities staff
- Emergency conditions accelerate burnout and turnover
Patient satisfaction, staff satisfaction, and compliance performance are tightly intertwined — and all are influenced by the reliability of critical systems.
Thin Margins Make Failure Risk a Financial Issue
Healthcare margins leave little room for error.
For nonprofit hospitals, studies show that for a 5% profit margin, which is very good, every $1 saved on energy costs is equivalent to roughly $20 in new revenue, once margins are considered.
That means:
- Unplanned energy waste and emergency repairs erode financial flexibility
- System failures don’t just cost money — they displace capital that could support patient care
Critical system failures convert predictable operating expenses into unpredictable financial shocks.
From Reactive Crisis to Preventable Risk
The hospitals that avoid these cascades don’t wait for failure. They shift from reactive maintenance to proactive risk management.
That typically includes:
- Identifying single points of failure in HVAC, steam, power, and controls
- Modernizing systems to restore redundancy and control
- Implementing monitoring that flags degradation before systems fail
- Funding upgrades through guaranteed operational savings rather than capital budgets
This approach reframes infrastructure from a sunk cost into a controllable risk lever.

A Better Way Forward
Hospitals don’t need more capital to reduce failure risk.
They need a strategy that aligns compliance, patient care, and financial performance.
CEG Solutions partners with healthcare organizations to identify critical system vulnerabilities and implement self-funded infrastructure upgrades using guaranteed energy and operational savings — without requiring upfront capital.
If your facility is operating aging critical systems, the most expensive outcome is waiting for failure to make the problem visible.
Talk to a CEG healthcare infrastructure expert to start with a no-cost assessment. You are already spending the money – let’s capture those costs and reinvest them back into your assets and return some to the balance sheet.

Related Posts
-
In energy-intensive segments like food processing, energy costs can account for 15 to 30 percent of total operating expenses. The challenge isn’t awareness….
-
59% of Students Say Sustainability Affects Where They Apply. Where Does Your Campus Rank? Survey data is reshaping how…
-
Deferred maintenance is often framed as a facilities problem: aging equipment, failing systems, or overdue repairs. But in…


